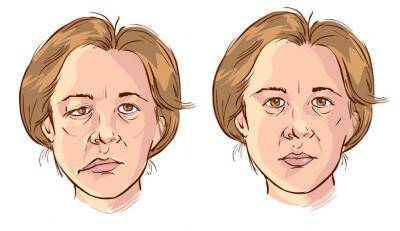
The facial nerve (nervus facialis) is the seventh nerve of the brain, which has several functions. Firstly, it acts as a motor nerve running to the mimic muscles of the face and thus determines your facial expression. The branch that runs to the tongue is responsible for the sense of taste (on the first third of the tongue). It is also involved in the operation of tear and saliva secretion. Facial nerve paralysis is slow to heal and can take up to a year. Although you usually get the first 5-10 treatments in a clinic, it’s not enough! You should continue the therapy at home until you are healed.
The facial nerve paralysis
Facial nerve paralysis is a paralysis of certain facial muscles, usually unilateral, innervated (innervated) by the facial nerve (n. facialis), especially the mimic muscles.
The facial nerve is the seventh (VII) of the twelve (XII) cranial nerves. It is paired, meaning that there is a facial nerve on the right and a facial nerve on the left. The cranial nerves originate from the nerve nuclei in the brain and run directly to the end organ (muscle, gland, etc.)
All the other nerves supplying the periphery (arms, legs and trunk) travel indirectly, which means they “switch” in the spinal cord and reach their destination from there.
The facial nerve supplies the mimic muscles (the platysma, one of the muscles of the forehead, eyes, nose, mouth and neck), the stapedius muscle in the auditory canal, parts of the “swallowing muscles”, as well as the anterior two-thirds of the tongue for taste perception (sensory) and almost all the glands of the head (visceromotor).
Forms of facial nerve paralysis
Due to the complex structure of the brain and nerves, damage can occur in many areas that can result in facial muscle paralysis.
Damage to the motor nucleus of the face (nuclear paresis) is rare.
Central paralysis
When the connection between the cerebral cortex and the motor nuclei in the brainstem (more specifically, the bridge (pons)) is damaged, it is called central or supranuclear paralysis. In this case, the central lesion is accompanied by other symptoms, such as paralysis of the arms or legs. The lesion causes contralateral (opposite side) damage to the mimic muscles, so the central lesion on the left side of the brain is represented by paralysis of the right side of the face. In the central form, it is mostly possible to frown and close the eyelids, due to the fact that the muscles of the upper half of the face are only two-thirds supplied by the opposite-sided facial motor nuclei and one-third by the right-sided facial motor nuclei (Hacke 2016). Thus, the muscles are weaker but still mobile.
Peripheral paralysis
The nerve is most often damaged below the nerve nuclei (infranuclear form). This is called peripheral facial nerve paralysis.
Symptoms of peripheral facial nerve paralysis always occur on the same side as the lesion (ipsilateral). Usually, the forehead and eyelid muscles are also affected. In addition, non-motor fibres may be affected, manifesting as taste disturbance and/or dysfunction of the salivary and lacrimal glands.
Causes of facial paralysis
Inflammation
Facial nerve paralysis can be caused by inflammation, in which case it is called facial neuritis. Here the peripheral nerve is affected by viruses or bacteria. Common pathogens are neurotropic viruses, herpes viruses and bacteria.
Central (brain) damage
Cerebral dysfunction leads to paralysis of the facial muscles, which can also have several causes: stroke (stroke, cerebral paralysis), multiple sclerosis, tumours, etc.
Peripheral lesions
Peripheral damage, specifically damage to the facial nerve itself, can be a cause of facial muscle paralysis.
- Idiopathic – i.e. the cause is unknown or cannot be determined. This accounts for 60-75% of cases (Finkensieper et al. 2012). In the remaining 25-40%, there are various underlying causes.
- Traumatic. Injury to the facial nerve leads to a fracture of the temporal bone.
- Damage. The nerve is encircled, compressed and compressed by the tumour. Different types of tumours can affect the nerve: parotid tumours, facial nerve schwannoma, acoustic neuroma, cerebellar tumours, meningitis caused by a tumour, etc.
- Iatrogenic (caused by medical intervention). Facial nerve damage may also occur as a possible complication of surgical removal of the parotid gland or subocular gland.
- As part of the following syndromes
Guillain-Barre syndrome (an acute inflammatory disease of the peripheral nerves), especially in Miller-Fisher syndrome (a variant of GBS)
Carey Fineman Ziter syndrome (congenital brain disorder)
Möbius syndrome (congenital malformation syndrome)
Melkersson-Rosenthal syndrome (inflammatory arterial disease)
Heerfordt syndrome (inflammation of the parotid and lacrimal glands) - Facial nerve paralysis can develop in metabolic diseases such as diabetes mellitus (especially if there is also hypertension)
- Also in pregnancy (especially in the last trimester) (Heckmann et al. 2017)
Depending on the cause, facial nerve paralysis may have more specific names:
- Bell’s facial paralysis: idiopathic (of unknown origin) facial nerve paralysis
- Ramsay Hunt syndrome: associated with zoster oticus infection
- Mona Lisa syndrome: paralysis during pregnancy
Symptoms of facial nerve paralysis
With the peripheral nerve usually affected on one side, the symptoms are usually unilateral, meaning facial nerve paralysis only affects one side of the face. Bilateral facial nerve paralysis occurs only in rare cases, for example in patients with Lyme disease.
The main symptom of facial nerve damage is paralysis of the mimic muscles:
- Small (drooping) mouth
- Twitching eyelids
- Brow furrowing not possible
- Eye muscle paralysis often makes it impossible to close the eyelids. There is a risk of dry eyes that requires symptomatic treatment.
In addition to the muscles, damage to the facial nerve can also affect other functions of the nerve:
- Decreased tear formation
- Sensitivity to noise (hyperacusis due to damage to the stapedius muscle)
- Diminished saliva production
- Impaired taste sensation (anterior two-thirds of the tongue).
- Pain, numbness or tingling in one side of the face is not due to facial nerve damage, but is sometimes due to the involvement of other nerves (trigeminal nerve) in some lesions.
The muscles on the intact side “pull” the damaged side, so your face becomes asymmetrical. You can’t move the muscles on the affected side, which gives you a mimicless expression.
Prognosis
Idiopathic facial nerve paralysis has a relatively good prognosis. In about 70% of cases, the paralysis resolves spontaneously within days or weeks, less often within months.
Only about 30% of people develop a permanent motor deficit (loss of mobility).
16% develop synkinesias, which include, for example, simultaneous involuntary movement of the eyes when the mouth is closed (Peitersen 2002).
First-onset unilateral facial nerve palsies also have a good prognosis, especially if the affected person is “young” (< 60 years old) and the nerve is only partially damaged (neurapraxia).
If the nerve is severely damaged or completely transected (axonotmesis), as in the case of a severe fracture of the petrous bone, complete resolution (remission) of symptoms is unlikely. If complete recovery is not achieved, it may more likely lead to facial asymmetry or synkinesia.
Paralysis of the muscles around the mouth is not only psychologically distressing but also limits everyday function. When drinking, the flabby muscles cause saliva or fluids to flow out of the corners of the mouth (“drooling”) or food to remain on the face. Reduced muscle strength can also affect speech. It can make it difficult to form sounds properly, making it harder to understand (dysarthria/speech impediment).
Symptomatic therapy and rehabilitation are particularly important for patients with severe injuries, permanent disabilities, and eating or speech problems.
Treatment of facial nerve paralysis
Always consider sudden paralysis of the facial muscles, whether peripheral or central, an emergency and seek medical attention immediately.
When the cause can be identified, the primary focus shifts to treating the underlying condition.
If the cause is unknown, the usual medication is steroids and/or antiviral drugs.
Symptomatic treatment may also be necessary. When the eyelid does not close, the use of artificial tears, eye ointment, and/or eye patches is employed to prevent the eye from drying out.
In cases of severe and persistent paresis, microsurgical techniques are sometimes used to reconstruct the facial nerve. This may involve utilizing the intact nerve on the opposite side (transverse facial nerve suture) or connecting it to other nerves (hypoglossal-facial anastomosis). Muscle grafting of the frontal muscle is also an option. As research continues, there are more and more options for surgical treatment.
Facial paralysis can be shocking, but the initial focus should be on rest and treating the underlying cause. It is important to drink plenty of fluids and rest. Avoid strain.
Electrotherapy and biofeedback
I have already written that in some cases paralysis will stop on its own. The problem is that it is impossible to know in advance who will be the lucky one who has a spontaneous resolution of paralysis after 1-2 months. Treatment should therefore be started as soon as possible.
You can also start electrotherapy treatment early, 3-4 days after the onset of paralysis. In most cases, people should persistently perform it for several months, and sometimes they may need to continue for up to a year. The regeneration of the nerve fibre is very slow, usually increasing by 0.1-0.2 mm per day, but even in the most optimal case only by a maximum of 1 mm. The length of the facial nerve can be 15-20 cm, so you can see from this that 150-200 days is the shortest possible.
You should do the electric treatment 2x-3x a day because the muscle that has lost its nerve fibre (called denervated muscle) atrophies in a short time without the impulses to move it. Eventually, the muscle will permanently deteriorate, overgrowing connective tissue, and you can’t improve from there.
With the electrical treatment of facial nerve paralysis at home, you can maintain the muscle in a functional state until the nerve fibre regrows and reaches the muscle again. Once the muscle is destroyed, the paralysis symptoms will no longer improve despite the regenerated nerve. However, if you find a muscle that is still intact, muscle function will return.
Central paralysis – ETS
For central paralysis of the facial muscles, functional electrical stimulation (EMG-guided electrostimulation), biofeedback or a combination of both is used to treat facial nerve paralysis at home. The exercises target one or more muscles (1 or 2 channels) and are designed to either restore function or prevent involuntary movements.
[message title=”Premium 400″ title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- Multifunctional electrotherapy device
- TENS | EMS, NMES, FES | MENS, MCR | Iontophoresis
- max. 4 channels (8 electrodes)
[/message]
[message title=”DuoBravo N – ETS – biofeedback-induced stimulation device” title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- EMG, electromyogram-based biofeedback

- ETS – stimulation “stimulation” on 2 channels
- central paralysis treatment, movement re-education, rehabilitation
[/message]
Peripheral paresis – denervated
For peripheral paresis, the emphasis is on treatment with special currents (low frequency, long pulse duration). The more significant the nerve damage – especially after surgical procedures – the emphasis is on electrotherapy to protect the muscles from atrophy (atrophy) and connective tissue disorders.
The misconception that stimulation prevents reinnervation (restoration of nerve function) has been disproved by recent studies (Carraro 2018). In fact, there is even evidence that low-frequency electrical stimulation promotes innervation (reestablishment of muscle-nerve contact) (Gordon et al. 2016).
As the healing process progresses and muscles become active again, synkinesia (simultaneous involuntary movements of the eye when closing the mouth, etc.) is often observed. Biofeedback therapy can help prevent these involuntary movements (Pourmomeny et al. 2014).
It is even more effective than mirror therapy alone (Dalla Toffola et al. 2012), although a combination with a mirror is certainly beneficial (Cardoso et al. 2008).
In general, stimulation can enhance motor functions, leading to good results (Bernd et al. 2018), as is the case with biofeedback therapy. It is also possible to use biofeedback for home-based treatment (Volk et al. 2014).
Find my article on how to treat facial nerve paralysis or bell’s palsy here.
[message title=”PeroBravo electrotherapy device” title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- an electrotherapy device

- denervated treatment – triangle, trapezoidal, square wave
- healthy muscle treatment – biphasic square wave
- ETS (EMG based) – biofeedback triggered stimulation
- time/intensity (i/t) testing support
- gait relearning function with foot sensor (peroneal paralysis)
[/message]
[message title=”Genesy 600 multifunction electrotherapy device” title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- multifunctional electrotherapy device

- TENS | EMS, NMES, FES | MENS, MCR | Ionto | Denervated
- max. 4 channels (8 electrodes)
[/message]
Soft laser treatment
You can use soft laser treatment at home as soon as symptoms develop to treat facial nerve paralysis, and it may be necessary to continue using it for several months.
You can read more about how to treat facial paralysis with soft lasers here.
[message title=”Personal Laser L400 soft laser” title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- 3. laser power class

- 808 nanometer laser beam
- CW (continuous wave) laser
- 400 mW power
- 12.5 sec / 5 Joule
[/message]
[message title=”EnergyLaser L500 Pro Soft Laser” title_color=”#ffffff” title_bg=”#1e73be” title_icon=”” content_color=”#000000″ content_bg=”#ededed” id=””]
- 3. laser power class
 808 nanometer laser beam
808 nanometer laser beam- CW (continuous wave) laser
- 500 mW power
- 10 sec / 5 Joule
- Android app – Bluetooth connection
[/message]
Treatments
The actual cause of facial nerve paralysis is that the nerve fibre (due to some effect) swells (becomes oedematous) and therefore the nerve fibre becomes “trapped” in the “bone tunnel” through the skull bone. When swelling causes the nerve fiber to press against the bone, it damages the nerve fiber, impairing its circulation and function.
Reducing nerve fibre oedema can minimise nerve fibre damage. Therefore, we recommend seeking treatment as early as possible following the onset of facial nerve paralysis.
Soft laser treatment stimulates microcirculation and improves blood circulation reducing oedema.
Soft laser treatment of facial nerve paralysis
Literature recommended for professionals: Aghamohamdi D, Fakhari S, Farhoudi M, Farzin H. The Efficacy of Low-Level Laser Therapy in the Treatment of Bell’s paralysis in Diabetic Patients. J Lasers Med Sci. 2020 Summer;11(3):310-315. doi: 10.34172/jlms.2020.52. epub 2020 Jun 21. PMID: 32802293; PMCID: PMC7369545.
Long term Treatments
Usually, hours pass before the diagnosis and initial treatment of facial nerve paralysis, causing some extent of damage to the nerve fiber. Another important effect of soft laser treatment is to help and support nerve fibre regeneration. You can read more about soft laser in my article.
Facial nerve paralysis is a permanent condition, so one should use not only use electrical treatments but also soft laser treatments over an extended period of time.
Devices suitable for the treatment of facial nerve paralysis are Personal Laser L400 and Energy Laser L500 Pro.